You’ve just created new life—now it’s time to reclaim part of your own. For many mothers, that means getting back into an exercise routine. Whether you ran throughout most of your pregnancy or want to pick up the hobby for the first time, learning how to begin running postpartum can feel overwhelming. Push yourself too hard too soon, and you risk delaying your recovery by weeks or could suffer a serious injury.
While I stopped running midway through my second trimester with both of my pregnancies, I was counting the days after delivery until I could start again. Even after a Cesarean section with my second, my body felt great after three weeks, and I was eager to reestablish my running routine. But I took the advice of my OB-GYN and held myself back. It took careful research and expert guidance from my health team to start again, and I’m running better than ever today because of it.
In this guide, we’ll break down some of the biggest questions and misconceptions about getting back into running postpartum so you can feel confident that your workout routine is making a positive difference for your body.

When Can You Start Running After Having a Baby?
If you’re struggling with the idea of taking time off, I know your pain.
First, take a breath. It’s easy to feel as if the weeks not running postpartum are wasted time, especially with the added pressure from society to “bounce back” after having babies. But the reality is that a few months off mean almost nothing long-term, and your body will be better for it.
Second, a disclaimer. Postpartum recovery looks different for everyone. When you’re physically recovered enough to start running depends on many factors, including the type of delivery, overall health before and after pregnancy, whether or not you’re breastfeeding, the state of your pelvic floor, and more.
Even your psychological state will have an impact, as some mothers use running as a coping strategy for postpartum anxiety or postpartum depression and consequently push themselves earlier and harder than they should.
Now let’s take a look at the specifics.
Until recent years, there’s been little consensus about when women can return to vigorous physical activity. That changed in 2019 with the publication of postpartum exercise guidelines endorsed by the Association of Chartered Physiotherapists in Sports and Exercise Medicine.
This article highlights the importance of waiting and easing back into exercise slowly to reduce the risk of serious injuries like including hernias, muscle tears, urinary incontinence, and pelvic organ prolapse.
“Running is a high-impact activity placing a lot of demand on your body,” the authors state. “To be run-ready, your body needs time to heal and regain its strength after having a baby. For this reason, we recommend following an initial low-impact exercise timeline, followed by a return to running between 3-6 months postpartum.”
This puts the timeline for running again at least twelve weeks after delivery. That’s twice as long as the six weeks often suggested at postpartum appointments.
Why the delay? It’s due in part to protecting your pelvic floor.
How Pregnancy Changes Your Pelvic Floor Region
It’s no secret that pregnancy affects your body—often permanently. Your pelvic floor is no exception. The musculoskeletal system becomes relaxed during the late stages of pregnancy as it adjusts to your increased hormone levels and overall weight.
Giving birth puts the pelvic floor at high risk of injury, and it can take between four and six months for it to recover fully—far longer than the six weeks of rest most doctors recommend.
The study recommends all women get evaluated by physiotherapists or pelvic floor specialists postpartum. They can help assess your current health and recommend pelvic floor exercises for restoring full functionality.
Am I Ready To Run? Signs You Need to Recover Longer.
The 12-week timeframe works for women who had healthy pregnancies and vaginal deliveries. Your body might require more time. Risk factors that affect your timeline include:
· C-section delivery
· Obesity prior to pregnancy
· Excessive scar tissue near the pelvis/ perineal tearing
· Diastasis recti (more on this later)
· Urine leakage when sneezing, coughing, or jumping
· Feelings of pressure in the pelvic area
· Low back pain or pain during intercourse
· Vaginal bleeding
· Swelling in the legs

How Do You Start Running After Having a Baby?
You’ve given your body a full three months to recover. Now, it’s possible to start adding running back to your routine. The key here is starting slow—overdoing it early on may set you back weeks.
As you settle back into an exercise routine, it’s important to keep the following objectives in mind.
Take a Strength Assessment
Growing a baby takes different muscles than you use in daily life. As such, you might not have a good sense of where you need to focus to get back into running. Meeting with a certified physical therapist for a checkup can help you get a sense of your baseline and learn where you could improve. For example, a physician may recommend physical therapy to focus on your glutes through single leg squats and calf raises which may make a difference in your functional fitness.
Prioritize Pelvic Floor Health
Research shows that high-impact exercises like running can increase your risk of pelvic floor dysfunction. Signs of problems include feelings of heaviness, moderate to severe pelvic pain, and urinary incontinence.
One way to improve your pelvic floor? Climb stairs. Going uphill is easier on the pelvic floor than downhill, giving your legs and core a chance to strengthen before you return to your full fitness routine.
Focus on Core Strength
Your core muscles take a beating during pregnancy, and it takes time postpartum to get them back in working order. A strong core stabilizes your body as you run, helping you maintain correct posture and reducing the risk of injury.
Ease into core work slowly. It’s best to start with moves designed for postpartum, such as leg extensions and bird-dog. Consider maintaining a habit of regular strength training long term. Even ten minutes of focused core exercises a few times a week will keep you strong.
Walk Before You Run
Fitness experts agree—the best way to ease back into running postpartum is to walk. Give your body time to reacclimate to itself sans baby with a walking routine that incorporates small amounts of running.
Keep your goals reasonable. Your first workout could consist of one to two minutes of running between five-minute walking intervals. As your fitness returns, you can lengthen the running intervals and shorten the walking time. A running coach can help you develop the best running program for your needs.
If you want to find a way to improve core strength and walk while the weather is warm, consider walks with a weight vest.
Should I Use a Jogging Stroller?
A jogging stroller is a baby registry must-have for pregnant moms. But don’t take yours for a spin on your first run during postpartum recovery. First, it’s best to wait until babies are between six and eight months old and can hold their heads upright.
Second, pushing a jogging stroller requires different muscles than running solo. Though research is limited, one 2017 study indicates that running with a jogging stroller leads to “minor changes in trunk, pelvis and hip kinematics.” If you plan to use one, take the time to perform flexibility work for the spine, pelvis, and hips to stave off injury.
If looking for a jogging stroller, consider this Amazon Baby Trend Expedition with over 13,000 4.7-star reviews.
Other Considerations for Returning to Running Postpartum
There’s a lot to account for as you ease back into exercise after having a baby.
Hormone Shifts
Your hormone levels are in for a wild ride when you have a baby. One minute you might be crying tears of joy at the tiny bundle in your arms; the next, raging that you don’t want anyone to touch you for the next two weeks.
The good news is that the extreme pendulum swings start leveling out around two or three months for most women to pre-pregnancy levels. In the meantime, give yourself grace and permission to feel how you do. This may be an intense stage, but it’s temporary. Your running routine can wait until you feel like yourself again.
Diastasis Recti
Diastasis recti is a separation of your “six-pack” muscles at the midline of your belly. It’s a common postpartum condition because the uterus stretches out your abdominal wall.
Returning to running before addressing it can slow recovery and worsen the separation. If you can fit one or more fingers between your abdominal muscles, seek out postpartum-safe strength-building exercises from a pelvic floor specialist.
Breastfeeding
Don’t let doubters tell you otherwise—running while breastfeeding is entirely possible. I’ve managed it for three years and counting.
Nonetheless, navigating a return to running while breastfeeding takes some planning. To start, you may need to time runs around your baby’s feeding schedule or be willing to pump immediately beforehand. A more supportive sports bra might be necessary to keep you comfortable.
Finally, consider that breastfeeding burns an estimated 500-700 calories per day and takes a ton of your body’s water supply. If you don’t adjust your hydration strategy and nutrient intake accordingly, you may fade fast during a workout.
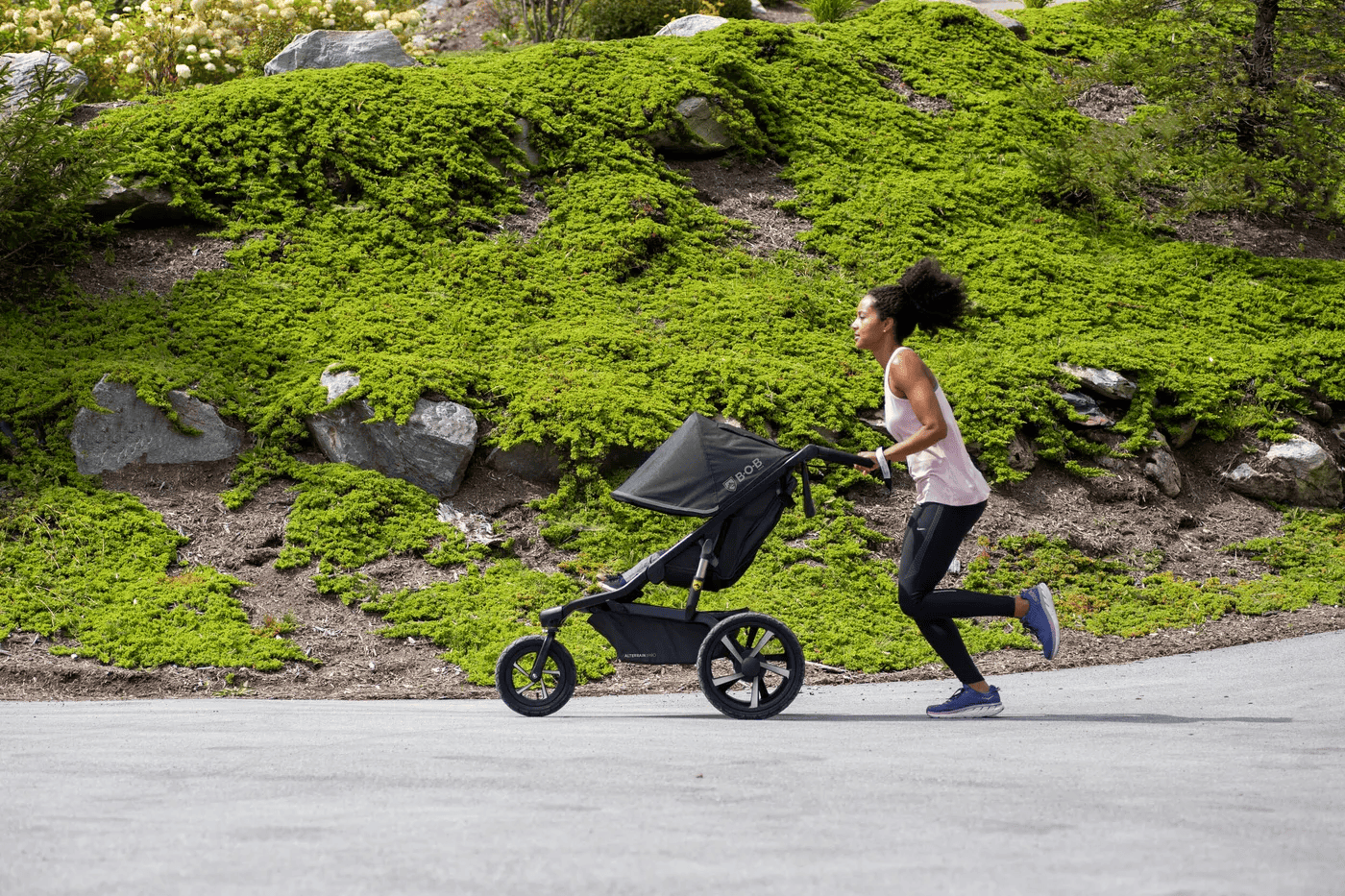
The Postpartum Running Checklist
- Listen to your body: Returning to pre-baby fitness is a (half) marathon, not a sprint. If your body needs more time, take it!
- Eat and drink wisely: Nutrients are at a premium right now for your body. Focus on eating healthy, whole foods, and drinking plenty of water.
- Invest in the right running gear: Feeling comfortable and confident in your clothes can make or break a workout. Check out our guide for must-have running gear for success. Pay extra attention to getting supportive running shoes to protect your looser ligaments.
- Get lots of sleep (or as much as you can): While you may be dealing with a baby waking you at every hour of the night, it’s important to prioritize rest to give your body adequate time to recover between workouts.
- Focus on your core and pelvic health: Weekly core exercises will improve your form and stability while reducing the risk of developing pelvic floor problems.
- Keep up fitness with cross-training: Mix biking or strength workouts into your routine, and try never to run two days in a row for the first weeks back.
- Up your iron: Creating and sustaining life takes a toll on your iron levels, so consider a daily supplement to keep yours up.
Running Postpartum Final Thoughts
Returning to running postpartum might feel overwhelming, but you can set yourself up for success. The key is to start slow—both in time and pace.
Give yourself a full twelve weeks to recover, and ease back into your routine with a mix of walking and running. Don’t be afraid to seek out expert guidance from medical professionals along the way. Taking the time to heal your body from the inside out can prevent problems in the long run (pun intended).
Most importantly, hold your goals loosely and give yourself grace for where you’re at—your body just did something incredible. It deserves all the time you can give it to recover.
Postpartum Running FAQ
No. The current medical consensus recommends waiting twelve weeks or longer before running.
Participating in high-impact activities soon after childbirth can worsen your pelvic floor muscles, potentially leading to pelvic organ prolapse.
Pregnancy and c-sections or vaginal delivery push the body in ways it’s unaccustomed to. It takes at least three months for things to heal.
Pain while running postpartum may be due to a weakened core, loose joints, pelvic floor issues, etc. It’s best to stop running and speak with a doctor if the pain doesn’t go away.
Having a baby impacts your pelvic floor and can weaken the muscles responsible for withholding urine. Performing kegels multiple times a day can help restore it.
Start slowly. Wait at least twelve weeks and begin by walking with short, slow bursts of running.
Every woman’s body is different. Whether or not you lose weight running depends on many factors beyond your fitness habits, including your weight before pregnancy, whether you are breastfeeding, and more.





